What are the Improvement Strategies?
The Improvement Strategies are an interactive knowledge management tool for primary health care (PHC) improvement. The Improvement Strategies are made up of a collection of modules aligned with the WHO-UNICEF Primary health care measurement framework and indicators.
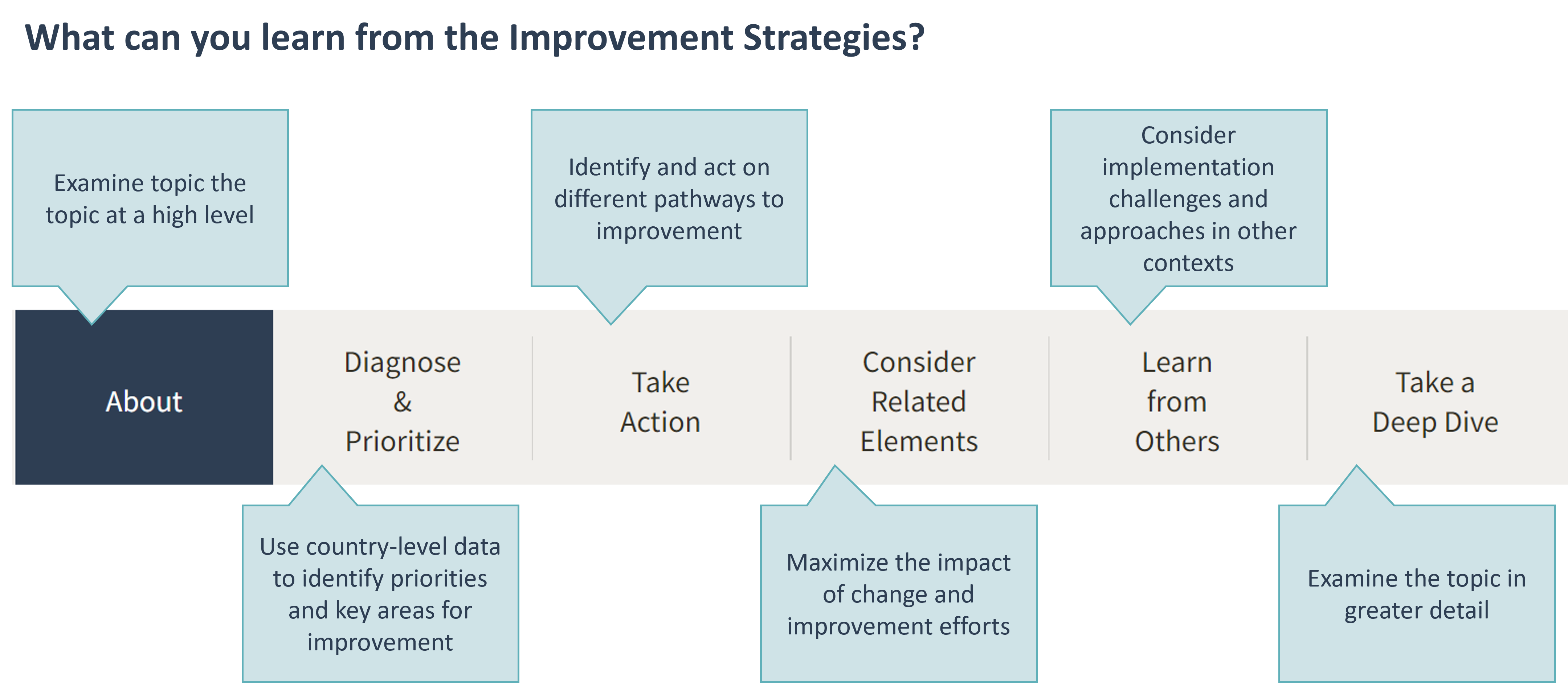
Each module addresses a topic that is critical for strong PHC capacity and performance and includes curated evidence on PHC improvement to help users identify appropriate strategies, relate these to other parts of the health system, and begin improvements. Within each module, users can navigate to the content most relevant to their role within the health system and country context. The sections in each module are designed to help country stakeholders:
- develop a nuanced understanding of topics relevant to strong PHC
- use this knowledge to being to plan and enact improvement efforts in their context.
The Improvement Strategies can be explored in any order. Please note the guidance and recommendations described within each of the steps are not inteded to provide a one-size-fits-all solution. Each step will need to be highly tailored to the unique needs and context of the country and/or local community to ensure success.